COVID-19 VACCINE FOR 6 MONTHS-AGE 4
COVID-19 VACCINE FOR 6 MONTHS-AGE 4
The use of the Moderna vaccine in children 6 months – 17 years is expected to be approved within the next week. Additionally, the use of the Pfizer vaccine is expected to expand to include children 6 months – 4 years old. If approved, West End Pediatrics supports your family’s decision to receive either the Pfizer or Moderna COVID vaccine.
At this time, we anticipate continuing to offer the Pfizer COVID vaccine to all patients 5 years and older because it is the only vaccine that has an approved booster dose. Additionally, we plan to offer both Pfizer and Moderna vaccines to children 6 months – 4 years.
While we expect to have enough vaccines to vaccinate all our patients, there are some limitations on how many daily dosages we can offer in our office. We will send out a mass email with details on scheduling. Stay tuned for updates.
How the Moderna-and-Pfizer-Vaccines-Work.pdf Vaccines WORK
The Pfizer and Moderna vaccines are both mRNA vaccines. This is a new type of vaccine that has not been used before. mRNA is the genetic material of the coronavirus. A small piece of the coronavirus mRNA that codes for its harmless ‘spike protein’ is injected. Our cells take-up this small piece of mRNA and use the code to manufacture the spike protein using our own cellular machinery. The protein is placed on the cell surface. Our immune system recognizes this spike protein as foreign and mounts an immune response against it. The end product of this immune response is antibodies against the spike protein. These antibodies help prevent infection from the actual coronavirus.
This is a very abbreviated and simplified description of the vaccine. If you are interested in learning more, the CDC has a nice summary of the process and a more detailed explanation below.
CDC.gov – Understanding mRNA vaccines
CDC.gov – Understanding how COVID-19 vaccines work
Does the coronavirus mRNA interact with our DNA?
No. The mRNA does not interact, affect, or get integrated in our own DNA in any way!
Is the vaccine safe?
Yes, the vaccine is safe. A group of more than 20 independent vaccinologists, immunologists, pediatricians, and other medical professionals thoroughly reviewed the data from the Pfizer and Moderna clinical trials. After that discussion, the group felt that the benefits of the vaccine far outweigh the risks of the vaccine and voted to approve both vaccines. Based on this review, the FDA granted Emergency use Authorization (EUA) for both vaccines. (note: I watched the FDA hearing personally and was very convinced that the vaccines are both safe and effective).
Here is a more in-depth discussion of the FDA EUA process:
FDA.gov – Emergency Use Authorization (EUA) explained
Are there side effects
Yes. As with most vaccines side effects are possible. The most common side effects for both vaccines are pain, swelling, and/or redness at the injection site. Fever, headache, and fatigue were also reported in a much smaller number of people. There are other very rare side effects, including a severe allergic reaction.
The CDC and the vaccine manufacturers have been very transparent with their data and the vaccine approval process. The FDA and manufacturers continue to collect data about safety and side effects. For more details, follow these links:
CDC.gov – Information on the Pfizer/BioNTech vaccine
CDC.gov – Information on the Moderna vaccine
CDC.gov – COVID-19 vaccine and severe allergic reactions
CDC.gov – What to expect after the COVID-19 vaccine
CDC.gov – Local, systemic, and allergic reactions to the Pfizer COVID-19 vaccine
Is the vaccine effective
Yes. The data shows that the both vaccines are very effective at preventing infection with the coronavirus and preventing serious illness with COVID-19. There is not enough data to determine if it helps prevent spread of the coronavirus from a vaccinated person to a susceptible person – which is why you should still wear a mask even after being vaccinated!
- How long does it take to work? – Both vaccines are two doses, separated by about three or four weeks. There is a high level of immunity starting about 1 week after the second dose.
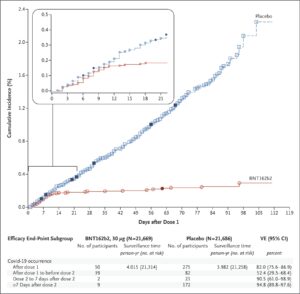
- How it was deemed to be effective? – A phase 3 clinical trials was conducted where about 50% of participants got the vaccine and 50% got placebo. COVID-19 infection rates were compared in the two groups. Those that got the vaccine were FAR less likely to contract COVID-19 (see the graph below)
- How long does immunity last? – We do not know. More studies are being conducted to answer this question.
Who will get the vaccine?
The vaccine is being distributed from the Federal Government to State Governments. Vaccine distribution decisions are made at the state and local level.
https://coronavirus.dcoronavirus.dc.gov
Can I get the vaccine if I am Breastfeeding
Breastfeeding mothers were not specifically studied in the vaccine trials so less data of safety and efficacy is currently available. However, The American College of Obstetricians and Gynecologists (ACOG) and other organizations have recommended that lactating women should have equal access to the vaccine and that breastfeeding is not contraindicated after getting the vaccine.
ACOG.org – Clinical Guidance for COVID-19 vaccine
CDC.gov – COVID-19 vaccine considerations for pregnant and breastfeeding women
Can I get the vaccine if I am pregnant?
Similar to breastfeeding, the vaccine studies did not look specifically at the safety or efficacy of the vaccine in pregnant women. However, ACOG has recommended that “COVID-19 vaccines should not be withheld from pregnant individuals who meet criteria for vaccination based on ACIP-recommended priority groups.” If you have specific questions, we recommend that you speak with your OB/GYN.